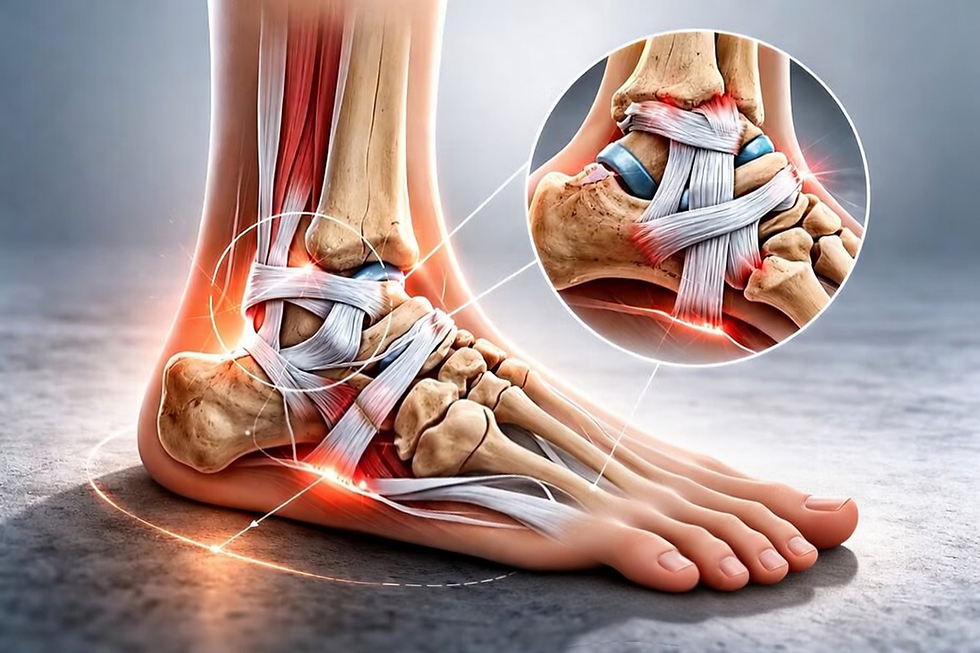
Arthritis in Ankles: Symptoms, Causes, and How Podiatry Can Help
- Sydney Allied
- Feb 23
- 9 min read
Updated: Feb 25
Ankle pain that doesn't go away, morning stiffness that makes your first steps feel difficult, or swelling that seems to linger long after rest — these are signs that shouldn't be ignored. For many Australians, these experiences are caused by arthritis in the ankles, a condition that can significantly affect mobility, comfort, and quality of life. While ankle arthritis is less common than arthritis in the hip or knee, it can be just as debilitating — and in many cases, it develops silently over years following an old injury.
At Sydney Allied Health Group, our podiatry team works with patients experiencing ankle arthritis to provide evidence-based, goal-oriented care that helps manage symptoms and support long-term function. Whether you are dealing with post-traumatic ankle arthritis, osteoarthritis of the ankle, or rheumatoid arthritis in the ankles, understanding your condition is the first step toward meaningful relief.
What Is Arthritis in the Ankles?
Arthritis is a broad term that refers to inflammation and degeneration within a joint. When it affects the ankle, it typically involves the tibiotalar joint — the main joint where the shinbone (tibia) meets the talus bone of the foot. As cartilage within this joint breaks down, bones begin to move with less cushioning and more friction, resulting in pain, swelling, and reduced range of motion.

Types of Ankle Arthritis
There are several types of arthritis that can affect the ankle joint, and understanding which type you have will influence your treatment pathway.
Osteoarthritis of the Ankle
Also referred to as degenerative joint disease, osteoarthritis involves the gradual breakdown of joint cartilage over time. Unlike hip or knee osteoarthritis, ankle osteoarthritis is less commonly caused by aging alone. Research indicates that in approximately 90% of cases, ankle osteoarthritis is related to a previous injury — making it predominantly a post-traumatic condition.
Post-Traumatic Ankle Arthritis
This is the most common form of ankle arthritis. It develops following a significant ankle injury — such as a fracture, severe sprain, or ligament tear — sometimes years or even decades after the initial trauma. The injury disrupts the mechanics of the joint, accelerating cartilage wear and increasing the risk of degeneration.
Rheumatoid Arthritis in the Ankles
Rheumatoid arthritis (RA) is an autoimmune condition that causes the immune system to attack the synovial lining of joints. The ankle is frequently affected in people with RA, often alongside other joints. Unlike osteoarthritis, RA tends to affect multiple joints symmetrically and is accompanied by systemic symptoms such as fatigue and generalized inflammation.
Gout
Gout is a form of inflammatory arthritis caused by a build-up of uric acid crystals in the joints. While it most commonly affects the big toe, the ankle joint can also be involved, causing sudden, intense episodes of pain, swelling, and heat.
How Do I Tell If I Have Arthritis in My Ankles?
FAQ How do I tell if I have arthritis in my ankles? Common signs include persistent ankle joint pain, morning stiffness lasting 20–30+ minutes, swelling and warmth around the ankle, reduced range of motion, a grinding or clicking sensation, ankle instability, and difficulty walking on uneven surfaces. A podiatry assessment with imaging is needed for a confirmed diagnosis. |
Recognizing the early signs of ankle arthritis can help you seek care before the condition progresses. Symptoms can vary depending on the type and severity of arthritis, but common indicators include:
Persistent ankle joint pain that worsens with activity or prolonged standing
Morning stiffness lasting more than 20–30 minutes after waking
Swelling and warmth around the ankle joint
Reduced range of motion, making it difficult to flex or rotate the ankle
A grinding or clicking sensation (crepitus) within the joint
Ankle instability or a feeling that the joint may give way
Pain that flares during weather changes or after periods of inactivity
Difficulty walking on uneven surfaces or navigating stairs
It is important to note that ankle pain does not always indicate arthritis — other conditions such as tendonitis, bursitis, or ligament damage can produce similar symptoms. A thorough clinical assessment by a podiatrist, including a review of your history, physical examination, and diagnostic imaging if required, is essential for an accurate diagnosis.
How Is Ankle Arthritis Diagnosed?
Diagnosis typically involves a combination of physical examination and imaging. Your podiatrist or referring clinician may order:
X-rays to assess joint space narrowing, bone spurs (osteophytes), and structural changes
MRI scans to evaluate cartilage integrity, ligament health, and soft tissue involvement — particularly useful in early-stage arthritis
Blood tests to rule out inflammatory or autoimmune conditions such as rheumatoid arthritis or gout
What Causes Arthritis in the Ankles?
Understanding the underlying cause of your ankle arthritis is essential for developing an effective treatment plan. The most common contributing factors include:
Previous ankle injury — fractures, severe sprains, and ligament tears are the leading cause of ankle osteoarthritis
Repetitive high-impact loading — common in athletes, labourers, or those with physically demanding occupations
Biomechanical abnormalities — flat feet, high arches, or gait irregularities that place excessive stress on the ankle joint
Excess body weight — additional load through weight-bearing joints accelerates cartilage breakdown
Autoimmune conditions — including rheumatoid arthritis, psoriatic arthritis, and lupus
Genetics — a family history of arthritis increases your susceptibility
Age — while not the primary driver of ankle arthritis, cartilage naturally thins with age
How Do You Treat Arthritis in the Ankle?
FAQ How do you treat arthritis in the ankle? Treatment is tailored to the type and severity of arthritis, and typically begins with conservative care: custom orthotics, appropriate footwear, activity modification, physiotherapy, and anti-inflammatory strategies. When conservative care is insufficient, corticosteroid injections or surgical options such as ankle fusion or ankle replacement may be considered. |
There is no single approach to treating ankle arthritis — the most effective management plans are personalized, evidence-based, and tailored to the type and severity of arthritis, your activity levels, and your individual goals. At Sydney Allied Health Group, our podiatry team takes a conservative, non-invasive approach as the first line of care. Book an appointment to discuss your treatment options.
Custom Orthotics and Footwear Modifications
One of the most effective and immediate interventions for ankle arthritis is orthotics therapy. Custom-made foot orthotics are designed to redistribute load, correct biomechanical imbalances, and reduce stress through the ankle joint. They can also help improve gait mechanics, which in turn reduces compensatory strain on the knees, hips, and lower back.
Appropriate footwear is equally important. Supportive, well-fitted shoes with cushioned midsoles, motion control, and adequate ankle support can significantly reduce pain during daily activities. High-top shoes and boots that stabilize the ankle may be particularly beneficial. Your podiatrist can provide specific footwear recommendations based on your foot type and arthritis severity.
Activity Modification and Load Management
Modifying how you move — not stopping movement entirely — is a key principle in arthritis management. High-impact activities that repeatedly compress and load the ankle joint, such as running on hard surfaces or prolonged standing on concrete, may need to be adjusted. Replacing these with lower-impact alternatives such as swimming, cycling, or walking on softer surfaces can help maintain fitness and mobility without exacerbating joint inflammation.
Anti-Inflammatory Strategies
Managing ankle joint inflammation is central to symptom control. Depending on your presentation, your treating clinician may recommend:
NSAIDs (e.g. ibuprofen or naproxen) — for short-term pain and swelling management, always used under medical guidance
Corticosteroid injections — directly into the ankle joint to reduce acute inflammation and provide temporary relief
Ice therapy — applied to the ankle for 15–20 minutes following activity to reduce post-exercise swelling
Anti-inflammatory dietary strategies — including increased intake of omega-3 fatty acids and reducing processed foods and refined sugars
Physiotherapy and Rehabilitation
Working alongside our podiatry team, physiotherapy plays a valuable role in ankle arthritis management. Targeted physiotherapy focuses on improving joint range of motion, strengthening the muscles that support and stabilize the ankle, and correcting movement patterns that contribute to excessive joint loading. In a multidisciplinary clinic like Sydney Allied Health Group, podiatry and physiotherapy work collaboratively to deliver a comprehensive treatment plan.
How Do You Treat Inflammation in the Ankle Joint?
FAQ How do you treat inflammation in the ankle joint? Evidence-based strategies include rest and elevation during flare-ups, compression bandaging, cold therapy (ice packs), corticosteroid injections for moderate-to-severe inflammation, and hyaluronic acid injections (viscosupplementation) for ankle osteoarthritis. PRP therapy is an emerging regenerative option. Your podiatrist will work with your GP or specialist to coordinate the most appropriate pathway. |
When ankle joint inflammation is the primary concern, treatment aims to reduce swelling, calm the synovial lining of the joint, and prevent further damage. Evidence-based strategies include:
Rest and elevation — during acute flare-ups to reduce fluid accumulation
Compression bandaging — to manage swelling and provide joint support
Cold therapy (cryotherapy) — to numb pain and reduce acute inflammation
Corticosteroid injections — for moderate-to-severe inflammation that does not respond to conservative care
Hyaluronic acid injections (viscosupplementation) — to improve joint lubrication in osteoarthritic ankles
Platelet-rich plasma (PRP) therapy — an emerging regenerative option using the body's own growth factors to support tissue healing
Surgical Options for Ankle Arthritis
Surgery is considered when conservative treatments have not provided adequate relief and arthritis is significantly limiting daily function. Common surgical options include:
Ankle arthroscopy — a minimally invasive procedure to remove bone spurs, loose bodies, or inflamed tissue within the joint
Ankle fusion (arthrodesis) — the surgical fusion of the tibiotalar joint to eliminate bone-on-bone pain; reduces movement but is highly effective at relieving pain
Total ankle replacement (arthroplasty) — replaces the damaged joint with a prosthetic implant, preserving more movement than fusion
Surgical decisions are made in close consultation with an orthopaedic surgeon and are tailored to individual patient factors, including age, activity goals, and overall health.
What Is the Best Exercise for Arthritis in the Ankles?
FAQ What is the best exercise for arthritis in the ankles? The best exercises combine range-of-motion work, strengthening, and low-impact aerobic activity. Recommended exercises include ankle circles, dorsiflexion and plantarflexion stretches, calf raises, calf stretches, towel toe curls, and resistance band exercises. Low-impact aerobic activities such as swimming, cycling, and elliptical training are also highly beneficial. Always consult your podiatrist or physiotherapist before beginning a new program. |
Contrary to what many people assume, staying active is one of the most beneficial things you can do for ankle arthritis. Exercise helps maintain joint lubrication, strengthens the muscles that support the ankle, improves proprioception (balance and positional awareness), and can reduce pain over time. The key is choosing the right types of exercise — low-impact, progressive, and ideally guided by a healthcare professional.
Recommended Exercises for Ankle Arthritis
The following exercises are commonly recommended for people managing arthritis in the ankles. Begin gently and stop if any exercise increases your pain. Always consult your podiatrist or physiotherapist before beginning a new exercise program.
Ankle Circles (Range of Motion)
Sit comfortably in a chair with your feet slightly elevated. Slowly rotate each ankle in a circular motion — 10 times clockwise, then 10 times counterclockwise. This helps maintain joint mobility and reduces stiffness.
Ankle Dorsiflexion and Plantarflexion
Seated with your feet flat on the floor, slowly flex your ankle by pulling your toes up toward your shin (dorsiflexion), then point your toes away from your body (plantarflexion). Repeat 10 times per foot. This promotes full ankle movement and reduces morning stiffness.
Calf Raises (Strengthening)
Stand behind a sturdy chair or bench for balance. Rise onto your toes slowly, hold for two seconds, then lower back down in a controlled manner. Repeat 10–15 times. Strengthening the calf muscles reduces the load transferred through the ankle joint during walking.
Towel Toe Curls (Intrinsic Foot Strengthening)
Place a small towel flat on the floor. Sitting in a chair, use your toes to scrunch and pick up the towel. Repeat 10–20 times per foot. This strengthens the intrinsic muscles of the foot, improving overall foot stability.
Calf Stretch (Flexibility)
Stand facing a wall with one foot forward and one foot back. Keep the back knee straight and heel on the floor, and lean gently into the wall until you feel a stretch through the calf and Achilles. Hold for 30 seconds, repeat three times on each side.
Resistance Band Exercises
Using a light resistance band looped around the forefoot, perform controlled dorsiflexion and inversion/eversion movements while seated. These exercises build ankle stability and are particularly beneficial in post-traumatic ankle arthritis rehabilitation.
Low-Impact Aerobic Activities
Alongside targeted ankle exercises, low-impact aerobic activities can significantly improve joint health and overall physical function. Recommended options include:
Swimming and aqua aerobics — reduces joint load while maintaining cardiovascular fitness
Cycling — promotes ankle range of motion with minimal impact
Walking on flat, even surfaces with appropriate footwear
Elliptical training
These activities support healthy weight management, which in turn reduces the mechanical stress placed on arthritic ankle joints.
When Should You See a Podiatrist for Ankle Arthritis?
Key signs you should book a podiatry assessment: Persistent ankle pain lasting more than a few weeks • Ankle swelling that does not resolve with rest • Reduced ability to walk comfortably or perform daily activities • Recurring ankle stiffness — particularly in the morning or after sitting |
Early intervention is key. The sooner ankle arthritis is identified and managed, the better the long-term outcomes. A podiatrist can assess your biomechanics, recommend appropriate footwear and orthotics, provide a targeted exercise program, and coordinate care with physiotherapists and medical practitioners as needed.
How Podiatry at Sydney Allied Health Group Can Help
At Sydney Allied Health Group, our podiatry team provides comprehensive assessment and management for patients living with arthritis in the ankles. We take the time to understand how your condition affects your daily life and develop a personalized care plan aligned with your goals — whether that is reducing pain, returning to sport, improving your walking tolerance, or simply getting through your day with greater comfort.
Our multidisciplinary model means that when your care requires input from physiotherapy or exercise physiology, that collaboration happens seamlessly within the same network. We are committed to evidence-based, patient-centered care that supports your long-term health and wellbeing — not just short-term symptom relief.
If ankle pain or stiffness is affecting your quality of life, we encourage you to book a podiatry assessment with our team today.